Revision Joint Replacement
Revision Knee Replacement
Revision knee replacement surgery involves replacing part or all of your previous knee prosthesis with a new prosthesis. Although total knee replacement surgery is successful, sometimes the procedure can fail due to various reasons and require a second revision surgery.
Disease Overview
The knee joints are lined by soft articular cartilage that cushion the joints and aid in smooth movement of the joint bones. Degeneration of the cartilage due to wear and tear leads to arthritis, which is characterized by severe pain.
Total Knee Replacement
During total knee replacement, the damaged cartilage and bone is removed from the knee joint and replaced with artificial components. Artificial knee joints are usually made of metal, ceramic or plastic and consist of the femoral component and the tibial component.
Indications
Revision knee replacement surgery may be advised to patients if they have one or more of the following conditions:
- Trauma to the knee joint
- Chronic progressive joint disease
- Increased pain in the affected knee
- Worn out prosthesis
- Knee instability or a feeling of giving way while walking
- Loosening of the prosthesis
- Infection in the prosthetic joint
- Weakening of bone around the knee replacement, a process known as osteolysis (bone loss)
- Stiffness in the knee
- Leg length discrepancy
- Fracture
Surgical procedure
Revision knee replacement surgery may involve the replacement of one or all of the components.
The surgery is performed under general anesthesia. Your surgeon makes an incision over the knee to expose the knee joint. The kneecap along with its ligament may be moved aside so that there is enough room to perform the operation. Then the old femoral component of the knee prosthesis is removed. The femur is prepared to receive the new component. In some cases the damaged bone is removed and bone graft or a metal wedge may be used to make up for the lost bone.
Next the tibial component along with the old plastic liner is removed. The damaged bone is cut and the tibia is prepared to receive the new component. Similar to the femur, the lost bone is replaced either by a metal wedge or bone graft. Then, a new tibial component is secured to the end of the bone using bone cement. A new plastic liner will be placed on the top of the tibial component. If the patella (kneecap) has been damaged, your surgeon will resurface and attach a plastic component. The tibial and femoral components of the prosthesis are then brought together to form the new knee joint, and the knee muscles and tendons are reattached. Surgical drains are placed for the excess blood to drain out and the incision is closed.
Risks and complications
Like all major surgical procedures, there may be certain risks and complications involved with revision knee replacement surgery. The possible complications after revision knee replacement include:
- Stiffness in the knee
- Infection
- Bleeding
- Formation of blood clots in the leg veins
- Injury to nerves or blood vessels
- Prosthesis failure
- Patella (kneecap) dislocation
- Ligament injuries
Postoperative care
Following revision knee replacement surgery, a Continuous passive motion (CPM) machine may be used to allow the knee joint to slowly move. The machine is attached to the treated leg which slowly moves the joint through a controlled range of motion, while you relax.
You can walk with crutches or a walker. You will be sent for rehabilitation within a couple days of surgery. A physical therapist will teach you specific exercises to strengthen your leg and restore range of motion to the knee. Your physical therapist will also provide you with a home exercise program to strengthen thigh and calf muscles.
Knee immobilizers are used when performing physical therapy, walking and while sleeping in order to keep the knee stabilized.
Revision knee replacement surgery is performed to replace failed knee prosthesis with a new prosthetic component. The surgery improves mobility and enables you to return to normal activities with a pain-free knee.
Revision Hip Replacement
Revision hip replacement is a complex surgical procedure in which all or part of a previously implanted hip-joint is replaced with a new artificial hip-joint. Total hip replacement surgery is an option to relieve severe arthritis pain that limits your daily activities. During total hip replacement the damaged cartilage and bone is removed from the hip joint and replaced with artificial components. At times, hip replacement implants can wear out for various reasons and may need to be replaced with the help of a surgical procedure known as revision hip replacement surgery.
Indications:
Revision hip replacement is advised in patients with the following conditions:
- Increasing pain in the affected hip
- Worn out plastic or polyethylene prosthesis
- Dislocation of previous implants
- Loosening of the femoral or acetabular component of the artificial hip joint
- Infection around the hip prosthesis causing pain and fever
- Weakening of bone around the hip replacement (Osteolysis)
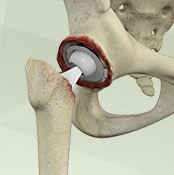
Revision hip replacement surgery is performed under general anesthesia. During the procedure, your surgeon will make an incision over the hip to expose the hip joint. Then the femur is dislocated from the acetabulum so that the old plastic liner and the metal socket can be removed from the acetabulum.
After removal, the acetabulum is prepared using extra bone and wire mesh to make up for the socket space and shape. Then the new metal shell is inserted into the socket using screws or special cement. A liner made of plastic, ceramic or metal is placed inside the metal socket.
To prepare the femoral component, the top of the femur bone is cut into several pieces to remove the implant. The segments of bone are cleaned and the new femoral implant is inserted into the femur either by a press fit or using bone cement. The segments of the femur and the femoral component are held together with surgical wires. Then the femoral head component made of metal or ceramic is placed on the femoral stem. All the new components are secured in place to form the new hip joint. The muscles and tendons around the new joint are repaired and the incision is closed.
After undergoing revision hip replacement, you must take special care to prevent the new joint from dislocating and to ensure proper healing. Some of the common precautions to be taken include:
- Avoid combined movement of bending your hip and turning your foot inwards because it can cause dislocation
- Keep a pillow between your legs while sleeping for 6 weeks
- Never cross your legs or bend your hips past a right angle (90 degrees)
- Avoid sitting on low chairs
- Avoid bending down to pick up things, instead a grabber can be used to do so
- Use an elevated toilet seat
Risks:
As with any major surgical procedure, there are certain potential risks and complications involved with revision hip replacement surgery. The possible complications after revision hip replacement include:
- Infection
- Dislocation
- Fracture of the femur or pelvis
- Injury to nerves or blood vessels
- Formation of blood clots in the leg veins
- Leg length inequality
- Hip prosthesis may wear out
- Failure to relieve pain
Revision hip replacement removes your failed hip implants from a previous total hip replacement surgery, and replaces them with new ones, which will help make your hip strong, stable and flexible again. It improves mobility, strength and enables patients to return once again to normal activity with a pain-free hip.

















